How Liver Diseases Progress
Your liver performs essential, life-sustaining functions
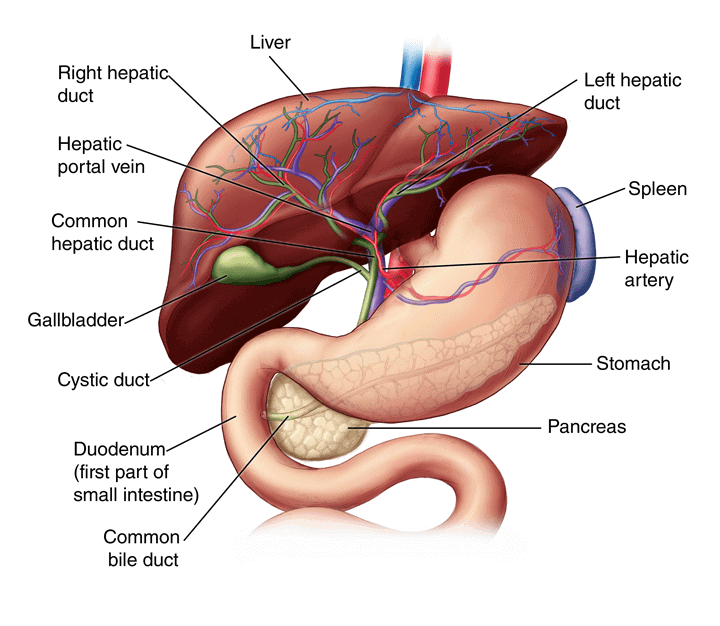
In America, liver disease affects millions and is on the rise. Did you know there are more than 100 different types of liver disease? Living with long-term, chronic liver disease can cause damage to your liver.
Learn more about clinic trial opportunities in your area.
Common Causes of Liver Disease
- Viruses
- Genetics
- Autoimmune disease
- Excessive use of alcohol
- Poor diet and/or obesity
- Reactions to medications, street drugs, or toxic chemicals
Most liver diseases damage your liver in similar ways and for many, the progression of liver disease looks the same regardless of the underlying disease.
Early Diagnosis of Liver Disease is Very Important
Early diagnosis may prevent damage from occurring in your liver. Your liver is an incredible organ. If you’re diagnosed when some scar tissue has already formed, your liver can repair and even regenerate itself. Because of this, damage from liver disease can often be reversed with a well-managed treatment plan.
Many people with liver disease do not look or feel sick even though damage is happening to their liver. At a certain point in the progression of liver disease damage can become irreversible and lead to liver failure, liver cancer, or death.
The Healthy Liver
We all need a healthy liver to live – it’s so essential that “live” is in the name!
Hepatitis (Inflammation)
While this controlled inflammation is essential to maintain proper function and balance in the liver, if it becomes dysregulated it drives the progression of liver disease. This diseased inflammation is called hepatitis.
Fibrosis (Scarring)
When someone has liver disease, their liver enters into a very dangerous cycle. Persistent inflammation, or hepatitis, sends nonstop signals to repair cells to continue depositing collagen. The extra collagen stiffens around the tissue like it is supposed to in the healthy liver; but, instead of a signal being released to stop the inflammation and discard the extra collagen, the inflammation continues, and even more collagen is deposited, leading to more stiffening. This is how fibrosis develops.
Cirrhosis (Severe Scarring)
Cirrhosis is where your liver is severely scarred and permanently damaged. While the word cirrhosis is most commonly heard when people discuss alcohol-induced liver disease, cirrhosis is caused by many forms of liver disease.
Liver Cancer
Liver cancer is cancer that begins in the cells of your liver. While several types of cancer can form in the liver, the most common type of liver cancer is hepatocellular carcinoma, or HCC, which begins in the main type of liver cells (hepatocytes).
Learn more about Liver Cancer.
Liver Transplantation
Liver transplantation is a surgical procedure performed to remove a diseased or injured liver from one person and replace it with a whole or a portion of a healthy liver from another person, called the donor.
Learn more about Liver Transplantation.
What to Ask Your Doctor
The best thing anyone can do for their health is to stay engaged in their healthcare. Be an active member of your care team by regularly visiting your healthcare provider, undergoing routine surveillance when needed, making the most of your appointments by asking questions and learning more about your health.
Learn what to ask your doctor.
Last updated on January 7th, 2025 at 11:53 am